Washington, DC
May 17, 2020
Hello readers,
I thought I’d share with you a few stories from the COVID ICUs.
Just after receiving Montréal Serai’s email in March asking for this submission, I admitted Mr. Jasper* into my ICU, an elderly African American man who had just come into the ER. As my fellow nurses were settling him in, I went to the conference/break/lunch room, away from the crowded scene, to get the ER nurse’s report. She told me several times that Mr. Jasper was her favourite patient ever, and described how chatty and nice he was despite having been sick for a few weeks and possibly suffering from a lack of care in the nursing home he came from. His oxygen had gone down in the ER, and they’d had to put him on a ventilator.
After our 10-minute briefing, we walked back to his room and noticed Mr. Jasper’s blood pressure and heart rate dropping. I grabbed a jet-fuel drug, and the last thing the ER nurse saw before she had to head back to the ER was me kneeling over this poor man’s bed, doing chest compressions. He survived our CPR, but the ER nurse didn’t know that.
I wondered how she felt ending her shift with such a shitty experience.
For me, the same kind of attachment to a patient occurred in a brief encounter seven weeks ago that lasted less than two minutes. I went into the room of Karina, a young-looking Latina woman in her forties, to borrow some equipment.
Karina was breathing through a facemask on 100% oxygen, lying prone on her stomach – a technique to help oxygenation. I asked her in my simple Spanish how she was doing, and she replied, “Bien gracias.” I asked her how her breathing was, and Karina smiled at me and cheerily replied, “Bien.” I left thinking she sounded too good to be in the ICU, unlike our other patients struggling to breathe. I cannot explain why I bonded with a patient after such a short visit, but it happens.
You know how they keep saying, “We’re all in this together?” We’re not. In this city that is now majority white thanks to relentless gentrification, our expanding COVID ICU beds are filled with blacks and Latinos, many of them in medically-induced comas on ventilators. While white workers are staying at home by themselves or in couples and telecommuting, it is the blacks and Latinos who comprise most of the essential workers, working in jobs with little protection and living in homes shared by many.
Four hours later, they were intubating Karina for the ventilator. The day after, she was transferred to the cardiac ICU to be placed on ECMO (extracorporeal membrane oxygenation) using a high-tech blood bypass machine, because her lungs were shot. A week later when I went to visit Karina, I was happy to see she had survived ECMO… most adult COVID patients do not. Yet she needed dialysis, as her kidneys had failed. Karina was still prone and sedated by our drugs. More than my other patients, her tragic fate really got to me. It finally made me realize that COVID-19 doesn’t play.
Karina ended up returning to a medical ICU, ventilated and in our drug-induced coma. She developed “COVID toes” that were turning gangrenous. But by last week, Karina had recovered enough to sit up in bed, was off most of the sedatives, and managed to weakly wave to me when I waved to her. I have visited her often, but I can’t tell if she remembers me. She now has a tracheostomy and looks rough to say the least – but what a force of nature she is, to survive this hell! So far.
Karina left the ICU a few days later. With a lot more luck, she will be able to rejoin her family and community.
And you know, through all of this the patients’ families are not allowed to visit except if their loved one is about to die. This is a very cruel disease exacerbated by our efficiency-driven health care.
We don’t have much to offer in the way of cures, yet we certainly are inflicting pain on families through our medical isolation protocols to prevent the spread of the virus. The marriage vow of sticking together till death do us part, and the bonds that make a family a family might be a natural result of our social DNA. Now hospitals and nursing homes are tearing it all asunder.
But tonight, nothing could break up the McBrides,* an elderly husband and wife team who were patients in the same room on a medical unit. At 17:29, Mr. McBride’s heart stopped due to oxygen starvation, and in rushed the code team to do advanced cardiac resuscitation.
The McBrides come from a home where their two children and Mrs. McBride’s mother also contracted COVID but recovered. For more than an hour, Mrs. McBride stayed in the room with her husband as he was worked on by the anonymous, gowned and masked code nurses, a respiratory therapist and doctors, who aggressively did CPR on him, shocked him, injected him with drugs and stuck tubes and needles into him to keep his heart from stopping, as it repeatedly did.
The code was successful in the most purely technical terms, as Mr. McBride somehow managed to get transferred to me in the ICU, with a beating heart on too much jet-fuel drugs. But clearly not long for this world.
How does Mrs. McBride feel seeing her husband’s repeated death and revival under the hands of a code team that swoops in performing our high-tech voodoo? It must be tragic and terribly frightening.
But I hope it’s not awful. I hope Mrs. McBride saw that we were fighting for Mr. McBride’s life when it mattered, honouring his wishes. That we cared. That we were present.
*Names have been changed to protect the patients’ identities.





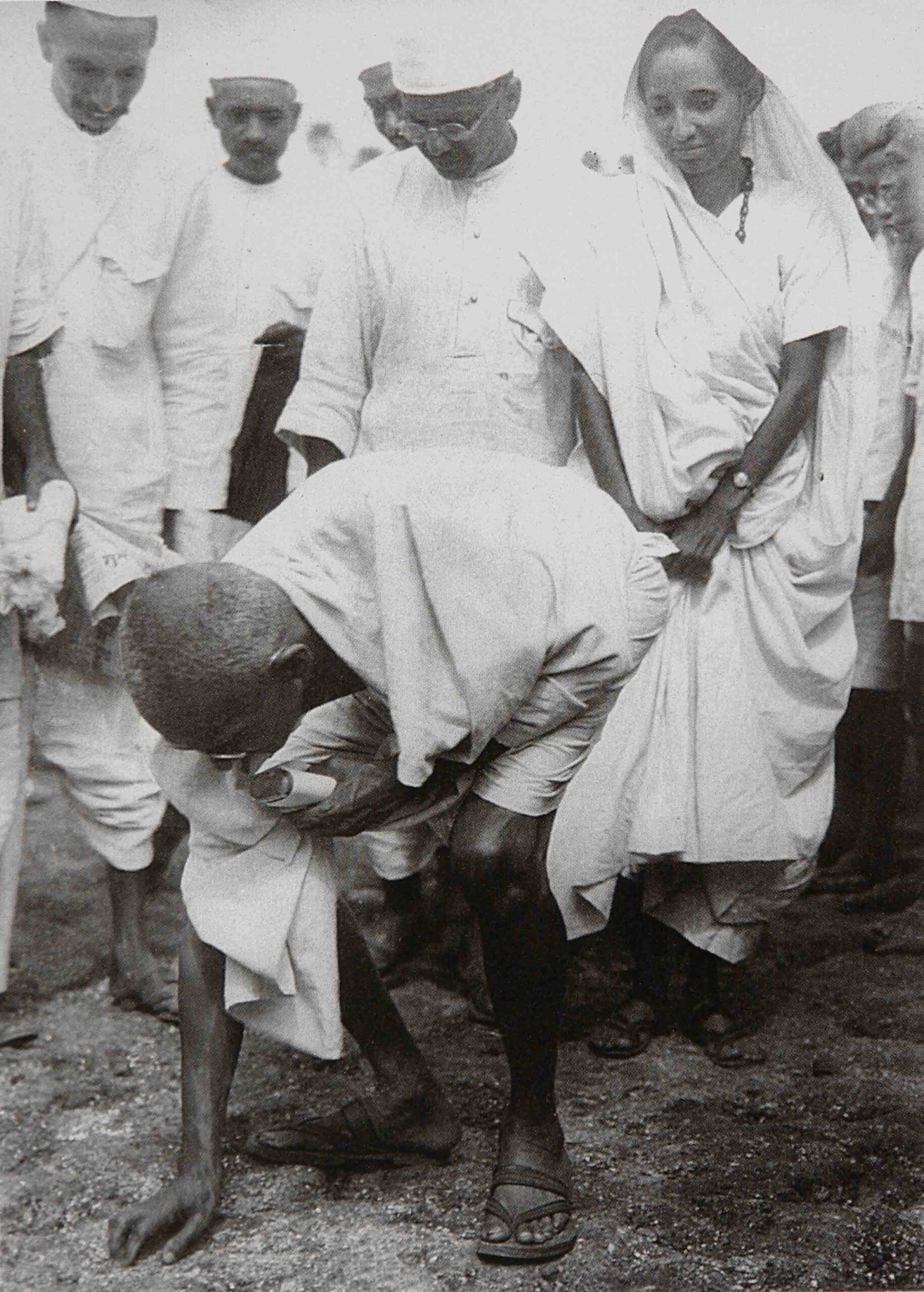



Thank you for this poignant letter, Scott. It’s very painful and sad to read. I agree that we are not all in this together, I don’t find the ubiquitous (in Québec) “Tout va bien aller” so appropriate in the context of all this suffering and dying, mainly experienced by the vulnerable: the residents in seniors’ homes, the socially marginalised,underpriviliged, and/or racialised. Thank (proverbial) god for the presence of all those dedicated health care workers, — you and your colleagues!